In the high-stakes world of United States healthcare, the difference between a thriving medical practice and one struggling with cash flow often comes down to a single administrative step: Insurance Eligibility Verification. While many providers view billing as a “back-end” process, the reality is that the revenue cycle begins the moment a patient calls to schedule an appointment. Failing to verify coverage at this critical juncture is the leading cause of claim denials, administrative burnout, and lost revenue.
At The Medicators, we have seen firsthand how transforming the front-end verification process can revolutionize a practice’s financial health. In this guide, we explore the multifaceted importance of verifying insurance before scheduling and how it serves as the ultimate safeguard for your revenue cycle.
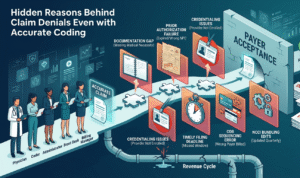
1. The Anatomy of a Claim Denial: Why Pre-Verification Matters
Statistics show that nearly 25% of all medical claim denials are related to eligibility and registration errors. These are “preventable denials.” When a patient is scheduled without a thorough benefits check, the practice risks:
- Expired Coverage: The patient may no longer be covered by the plan on file.
- Out-of-Network Status: The provider may not be in the patient’s specific network tier.
- Missing Authorizations: Many procedures require a “Prior Auth” that must be initiated days before the visit.
By implementing a “Verification-First” policy, The Medicators helps practices achieve a Clean Claim Rate (CCR) of 95% or higher. When the data is accurate at the start, the payment follows at the end.
2. Elevating the Patient Experience through Financial Transparency
The modern patient is also a consumer. With the rise of High-Deductible Health Plans (HDHPs), patients are responsible for a larger portion of their medical bills than ever before.
If a patient receives a surprise bill three months after an appointment because their insurance didn’t cover a service, it damages the provider-patient relationship. Pre-verification allows your staff to say: “Based on your current plan, your estimated out-of-pocket cost for today’s visit will be $45.”
This transparency:
- Increases Point-of-Service (POS) collections.
- Reduces the need for aggressive debt collection later.
- Boosts patient satisfaction and online reviews.
3. Optimizing the Revenue Cycle Management (RCM) Lifecycle
Revenue Cycle Management is a delicate ecosystem. A bottleneck at the beginning creates a “domino effect” of inefficiency.
Reducing Days in Accounts Receivable (AR)
When eligibility is verified upfront, claims move through the clearinghouse without friction. This reduces your “Days in AR,” meaning money enters your bank account faster. Practices that bypass this step often spend weeks chasing “Requests for Information” (RFIs) from payers, which stalls cash flow.
Streamlining Provider Workflow
Physicians want to focus on clinical outcomes, not billing disputes. When RCM services include robust pre-verification, the clinical staff doesn’t have to deal with the frustration of “non-covered” services after they have already dedicated time and resources to a patient’s care.
4. The Hidden Costs of Manual Verification
Many practices attempt to handle verification manually by having receptionists call insurance companies or log into individual payer portals. This is incredibly labor-intensive and prone to human error.
The Medicators utilizes advanced automated tools and dedicated specialists to perform real-time verification. This ensures:
- Coverage for the specific Date of Service (DOS).
- Detailed Benefit Breakdowns: Understanding co-pays, remaining deductibles, and co-insurance.
- Coordination of Benefits (COB): Identifying which insurance is primary and which is secondary.
5. Overcoming the “Competitor Gap.”
In the competitive landscape of California and Texas healthcare markets, top-tier practices are outsourcing their front-end tasks to specialized firms. If your competitors are using a professional service like The Medicators, they are operating with lower overhead and higher collection rates.
To stay compatible and competitive, your practice must shift from a “reactive” billing model to a “proactive” one. This means treating eligibility as a prerequisite for scheduling, not an afterthought.
6. How The Medicators Transforms Your Practice
At The Medicators, our mission is to eliminate the administrative burden that prevents doctors from being doctors. Our Medical Billing Services are designed to act as an extension of your office.
Our Verification Process Includes:
- Identity Confirmation: Ensuring the patient’s demographic data matches the insurance record.
- Benefit Validation: Confirming the specific service (CPT code) is a covered benefit.
- Authorization Management: Tracking and securing necessary referrals or prior authorizations.
- Real-Time Reporting: Providing your office with a daily “Eligibility Report” for all scheduled patients.
Final Thoughts: The Path to Financial Stability
The healthcare industry is moving toward a model where data accuracy is the only way to ensure profitability. By prioritizing Eligibility Verification Before Scheduling, you are protecting your practice from the volatility of the insurance market.
Don’t let “preventable denials” eat away at your hard-earned revenue. Partner with the experts who understand the nuances of the US healthcare system.
Ready to optimize your revenue? Contact The Medicators today for a free audit of your current billing workflow and see how we can help you achieve a 99% claim acceptance rate.
Frequently Asked Questions (FAQs)
Q1: What is the difference between eligibility verification and insurance authorization?
Eligibility verification confirms that the patient has an active policy and determines the extent of their benefits (co-pays/deductibles). Insurance authorization (or prior authorization) is a specific “green light” from the payer that they agree a particular procedure is medically necessary and will be covered. Both are essential, and both should be handled before the appointment.
Q2: How far in advance should we verify a patient’s insurance?
Ideally, verification should occur 48 to 72 hours before the scheduled appointment. This provides enough time to contact the patient if there is an issue with their coverage or to secure a last-minute authorization. For same-day appointments, real-time automated verification is a must.
Q3: Why did a claim get denied even though we verified the insurance?
Insurance verification is a “snapshot” in time. A policy might be active on Monday but terminated on Tuesday. Furthermore, “Verification” does not always guarantee payment; the claim must still be coded correctly. This is why a comprehensive partner like The Medicators is vital for us to manage both the verification and the complex coding that follows.
Q4: Does eligibility verification help with Medicare and Medicaid patients?
Absolutely. Medicare and Medicaid eligibility can change monthly. Verifying “MBI” (Medicare Beneficiary Identifier) numbers and checking for Managed Care or “Replacement” plans is critical to avoid the common “Wrong Payer” denial.
Q5: Can outsourcing verification actually save my practice money?
Yes. When you calculate the cost of staff hours spent on the phone with payers, the cost of denied claims, and the loss of revenue from uncollected co-pays, outsourcing to a specialized billing firm typically pays for itself through increased collections and reduced administrative overhead.