In the complex landscape of healthcare billing, small administrative oversights can lead to massive financial hurdles. For many clinics, the difference between a thriving practice and one struggling with cash flow is Insurance Eligibility Verification.
By confirming a patient’s insurance details before care begins, healthcare providers can stop billing problems before they start.
What is Insurance Eligibility Verification?
At its core, eligibility verification is the process of validating a patient’s insurance status and benefits prior to treatment. This proactive check ensures that:
- The patient’s insurance is currently active.
- The specific patient is covered under the plan.
- The requested medical service is a covered benefit.
- The exact copay or deductible amount is identified.
- Necessary prior authorizations or approvals are secured before care begins.
The High Cost of Claim Denials
A claim denial occurs when an insurance company refuses to pay for a service. When this happens, the clinic must dedicate time and money to fix the error and resubmit the claim, delaying essential revenue.
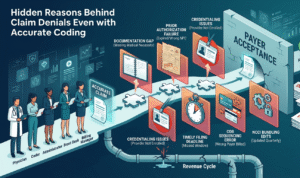
Common Reasons for Denied Claims
Many denials stem from simple, preventable mistakes:
- Wrong Patient Name: Data does not match insurance records.
- Expired Coverage: The policy is no longer active.
- Incorrect ID Numbers: The member number was entered incorrectly.
- Missing Approval: The treatment required prior authorization that was never obtained.
- Billing Code Errors: Using the incorrect medical code for a procedure.
How Verification Stops Denials and Boosts Revenue
Implementing a robust verification process helps clinics send “clean claims” submissions with zero mistakes that get paid much faster.
- Finds Mistakes Early: Verification allows staff to catch misspelled names or wrong birthdays before the billing phase.
- Validates Coverage Limits: Some plans do not cover every service; knowing this upfront prevents payment disputes.
- Secures Prior Authorizations: Verification alerts the clinic if a treatment needs approval first, ensuring compliance with payer rules.
- Checks Active Status: Because insurance can change at any time, verifying status ensures the plan hasn’t been terminated.
Manual vs. Automated Verification: Which is Best?
| Feature | Manual Verification | Automated Verification |
| Method | Phone calls and individual websites | Software-driven instant checks |
| Speed | Slow and labor-intensive | Fast and real-time |
| Accuracy | Higher risk of human error | Highly accurate |
| Cost | Low entry cost, high labor cost | Initial setup fee, lower long-term cost |
While manual checks might work for very small clinics, automation is the gold standard for modern practices looking to save time and reduce errors.
Best Practices for Practice Success
To maximize your Revenue Cycle Management (RCM), follow these industry best practices:
- Verify Before Every Visit: Insurance status can change overnight; never assume a patient’s coverage is the same as their last visit.
- Utilize Real-Time Tools: Use software that provides instant updates to minimize data entry mistakes.
- Invest in Staff Training: Ensure front-desk workers understand the importance of collecting accurate ID cards and updating records.
- Check Authorizations Early: Identify services requiring approval days before the patient arrives.
Transform Your RCM with The Medicators
Streamlining your billing operations doesn’t have to be a burden. The Medicators provides full-cycle RCM services designed to reduce payer denials and enhance collections.
By blending robotic process automation with machine learning, we solve the most challenging billing problems while integrating seamlessly with your current software. Our mission is to save you money and boost your income through precision and dedication.
Ready to lower your denial rate? Visit The Medicators to learn how we can help your clinic achieve a 95%+ clean claim rate.
Frequently Asked Questions (FAQs)
Why is eligibility verification important?
It is the most effective way to stop billing mistakes and prevent claim denials before they happen.
Can verification help clinics get paid faster?
Yes. By ensuring claims are “clean” and error-free, insurance companies approve and pay them more quickly.
Does this process help patients?
Absolutely. It helps patients understand their costs upfront and avoids “surprise bills” after treatment.
Should we verify insurance on every visit?
Yes. Insurance details and coverage rules can change at any time, making frequent checks essential.